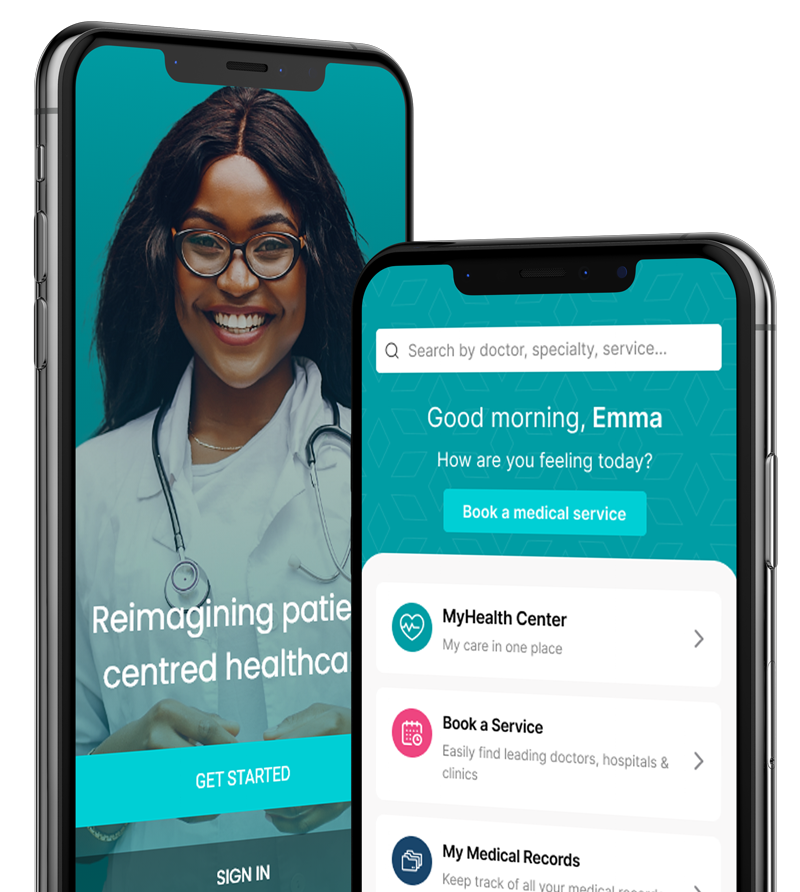
Access Top-Tier Specialised Healthcare Services Globally
Discover personalised medical solutions by connecting with the top medical specialists and facilities worldwide
Search for a medical service
Patient-Centric Services Tailored for You
Need help or have questions? Click the button below to speak to
a
caring support specialist who will guide you through our services.
Connect
with a support specialist now
Our Mission
Connecting patients to world-class medical care through our trusted hospital network42,000+
Patients Assisted1,500+
Medical Professionals100+
Hospitals2
Emergency Evacuation Partners
42,000+
Patients Assisted1,500+
Medical Professionals100+
Hospitals2
Emergency Evacuation PartnersYour Health Matters: Making Quality Healthcare Accessible for All
As a global healthcare facilitator, we are dedicated to offering our patients top-notch, safe, and affordable medical services.
Our team of seasoned medical experts, combined with an extensive network of hospitals and clinics worldwide, ensures that you receive the highest standard of care, no matter where you are.
Why Choose Us
- We cater to local and international medical needs
- 24/7 patient support
How We Do It
- We get you a free customized treatment plan
- We connect you with the leading hospitals and specialists

How Can You Access Our Healthcare Services?
-
Search and Select a Service
Looking for a doctor? Just search for the medical service you require. -
Book Your Appointment or Request a Service
Conveniently pick your desired date and time for the appointment. -
Receive Help from your Dedicated Patient Specialist
Our committed patient support team will guide you throughout your appointment. -
Attend Your Doctor's Appointment and Start Your Journey to Wellness
Visit the doctor and take the first step towards your improved health and well-being.

Medical Tourism
Helping you access high-quality care worldwide.

Care Beyond Borders
- Cost Savings
- Pair Treatment with Exploration
- Access to Highly Specialised Treatments
- Exceptional Quality of Care
Our Partner Hospitals Accept Some of The Leading Insurances Globally
Looking to receive treatment through your insurance provider? Our expert insurance team is eager
to assist.
Book
a service with
insurance
Seeking treatment through your insurance provider? Our expert team is here to help.
- Global Coverage Our collaboration with top insurance partners ensures extensive coverage that's accepted globally.
- No Additional Cost Our committed specialist team supports you at every stage, at no additional cost.
- We Facilitate Unlisted Providers For unlisted insurance providers, we're ready to help you find the right coverage. Inquire today.
Our Patients' Heartfelt Stories
Authentic reviews from satisfied patients - we're committed to delivering top-quality medical care and coordination for every treatment.
-
Naser
Multiple Health Issues, UAE “I would like to special thanks Doreen for her help and support during our time in Thailand, especially with the hospital (Bumrungrad International Hospital) and accommodations.” -
Josephine
Spinal Decompression Surgery, Kenya “Your services to us were very efficient, through and through. you linked us with the Surgeon at the Apollo Hospital in Mumbai in a record time; treatment estimates were very good and economical; your speed of giving feedback was excellent; follow-ups were exceptional. Airport pickup in India was very, very good.” -
Mohammed
Surgery, Bangladesh “Surgery was done quickly (at Bumrungrad International Hospital). After surgery I can walk without pain. Overall services is excellent, thanks doctors and nurses.”































































































































































































































.jpg)



.jpg)

.jpg)



.jpg)



.jpg)

.jpg)







.jpg)







![Delaware American Life Insurance Company [Metlife]](https://my1healthstorage.blob.core.windows.net/my1health/insurances/Delaware American Life Insurance Company [Metlife].jpg)

.jpg)

.jpg)












.jpg)



.jpg)








.jpg)
.jpg)



.jpg)
.jpg)
.jpg)
.jpg)

.jpg)



.jpg)
.jpg)







.jpg)




.jpg)








.jpg)





.jpg)
.png)